Agatha told me to practice bearing down until they were ready for me to start really pushing. I had no idea how to bear down without pushing, so I just pushed! Each time a contraction started, I lifted my shoulders, tucked my chin into my chest, pulled in my left leg - Jonathan had to move my right leg for me, I still couldn't feel it - and pushed as hard as I could for ten seconds at a time. After entering some data into the computer, Agatha came over to see how we were doing. She commented that my pushing was very effective. I interpreted that to mean our son was on his way down and out, and we would be done with this soon. We continued our routine, getting in 2-3 pushes per contraction. She encouraged me not to do more than that so as not to exhaust myself too quickly. Periodically she came over to check my progress, then went back to the computer. Each time I asked if he was getting any closer, and she would encourage me to keep going, that he would be here soon. During this time Dr. Partida was getting some rest herself; she had several of us in labor that night, and in between jumping from patient to patient she tried to recover some of her energy. She was wonderful, though, in that she never once made us feel like we were inconveniencing her or disrupting her time.
Speaking of time, it continued to move on as I pushed, breathed, pushed, rested; pushed, breathed, pushed, rested; etc. I still asked Agatha how well I was pushing, if I was making progress, every time she came to the bed. An hour went by, then another half an hour, then another. Jonathan later told me that it was painful to see me exerting so much effort and energy as Caleb's head would start to descend a little bit, but as soon as the pushing was over, he went right back up. There was no two steps forward and one step back, as birthing usually goes. It was two steps forward and two steps all the way back each time. Neither of them told me this at the time, though, and I appreciate that. I'm sure it would have been quite discouraging in the moment.
After about 1.5 hours of pushing, Dr. Partida came in to check on me and watch me push through a contraction. She agreed that I was effective and directing my pushes well, but he wasn't descending like he should be. The hospital's policy is to allow women to push for 2-2.5hrs before moving to a c-section. We had discussed this previously with her at a regular checkup, and she assured us that as long as mama and baby are handling labor well, she isn't one to enforce that policy. At this point, though I had been pushing for a while, the baby and I were both quite stable so we continued with the pushing.
Poor Jonathan was so good to me throughout all of this time. Of course no one gets more exhausted during this time than the mother, but it's exhausting to a degree for the support person, too. It was emotionally taxing on him to watch me struggle to get this baby out to no avail, not to mention he had to keep his energy up to encourage me and count with me and stay positive with each contraction. After a contraction was over I would lower my left leg, but he had to keep holding my right leg since it was just dead weight to me. Even though it had no sensation, I felt like it had to be held at just the right height. If he wasn't paying attention and lowered it even an inch I would scold him and ask him over and over to PLEASE keep it where it was! After the fact I realized how ridiculous it was, but in my mind it just wasn't comfortable to be held anywhere other than where I wanted it. He was a great sport and never gave me grief about harping on him about it.
After 2.5 hours I noticed that the feeling in my abdomen was changing with the contractions. As mentioned, there was a spot in my lower left abdomen where I could feel the tightening of each contraction. Now I felt that spot growing and some pain accompanying the tightening. Over the next 30 minutes, as I continued pushing, the pain intensified. I knew the epidural had nearly worn off and I was beginning to panic. I was absolutely unprepared to birth this baby without pain medication. Dr. Partida came back in to check my progress and I immediately informed her of my discomfort (to say the least). I begged them to do something, as by this point I had been pushing for 3 hours and strongly doubted my ability to continue without pain relief. My sweet doctor said they would have the anesthesiologist come back in, and to continue pushing in the meantime.
In between contractions I was extremely uncomfortable, but every time I pushed I felt immense relief from the pain and pressure. It felt SO good to push into the pain. Then I would stop pushing, take a deep breath, and all the pain and pressure came rushing back. Resume pushing, resume relief, pushing over, overwhelming discomfort returns. This is how it went for some amount of time - I'm not sure how long - until the anesthesiologist returned. He gave me a boost of the numbing agent in the epidural. I soon felt the warm relief creep in, but to my dismay I was more numb than before and could no longer feel even the tiniest bit of contracting. This meant I now needed someone to hold my left leg for me, and we had to rely on the monitor to tell us when I was contracting. I was so disappointed to no longer use self-directed pushing, not to mention I had a harder time directing my pushing effectively. I felt a little bit woozy and drugged, which I hadn't felt when I originally received the epidural.
After I was numbed back up, Dr. Partida returned to check on me. It had now been 3 hours and 15 minutes of pushing and she could see I still was not making progress. Throughout that time we'd been shifting me onto my right side, then onto my left, and back to the center, and nothing was making a difference. She agreed to give me half an hour to keep pushing on my own, and after that if he hadn't crowned, we would have to either try the vacuum or go for a c-section. We told her that a section was absolute last resort, and we'd be willing to try the vacuum first. Well, I was not about to get cut open if I had anything to say about it, so I bore down harder than ever during those next 30 minutes, determined to get this baby boy out on my own. But wouldn't you know, things just weren't lining up. She promptly returned, watched me push again, and said, "Ok, let's get the vacuum ready."
While the room was basically prepared for a birth, there were still a few things left to do. Another nurse brought in a warming station and blankets. (Our families were still in the waiting lounge at the end of the hall during this time, and they knew by the warmer that we were close.) Dr. Partida suited up in her delivery scrubs and someone prepared a small table with the vacuum suction, clamp, scissors, etc. Dr. Partida suspected the cord was around the baby's neck and had paged a team from the NICU to come in, just in case. (In hindsight, I believe she must have seen a series of heart decels on the baby's monitor.) Finally she was seated and ready to go with the vacuum. The moment of truth was here; would we be able to get him out vaginally, or would I be whisked away for a section? I was NOT having that, so I brought my a-game and mustered everything I had.
I didn't want a mirror so I have no idea what was going on down there. (And based on what Jonathan later told me about it, I'm glad for that.) Dr. Partida and I worked together as a team, me pushing and her pulling with the suction. The energy in the room intensified as we gradually got closer to getting his head out. At one point she said, "Okay Jessica, I want you to push as hard as you can. Keep pushing, don't stop!" So I squeezed my eyes shut and used every fiber in me to focus on pushing. After the usual 10 seconds, she said, "Keep going! Keep going!" So I quickly drew a breath and continued with the push. His head was so close, she didn't want us to lose all the progress we had made, so I continued with one huge push for about 30 seconds, taking gulps of breaths when I could. I felt myself losing ground; I was pushing so hard I couldn't hold my breath in any more. My throat and lungs didn't want to cooperate with all the pressure I was exerting. Just when I thought I had nothing left, his head emerged. Dr. Partida's instincts were right and the cord was wrapped around his neck. She quickly looped it around to pull it off, suctioned his nose and mouth, and in another push or two his body slid out. At 3:27am, 4 hours from the time I started pushing, our Caleb James was born. Our plan had been for Jonathan to cut the cord. Caleb was quite pale and not crying when he came out. Jonathan asked if he would be able to do that still, and she handed him the scissors and told him he could but had to do it quickly, so he did.
At this point my memory gets a little hazy. I was utterly exhausted, still feeling druggy from the epidural boost and oblivious to much of what was happening around me. I do remember a flurry of activity throughout the room. We had written in our birth plan for Caleb to be immediately placed on my chest after the birth, but because he still hadn't cried out, he was rushed over to the warmer where the NICU team suctioned him some more, covered him in towels and rubbed him to stimulate crying which would help clear out his lungs. Finally he let out a squawk and everyone breathed a deep sigh of relief. As soon as he did that they brought him over and placed him right on my chest. He was incredibly pale, almost pure white, and continued to be fairly quiet. We rubbed him, stroked his arms, talked to him, encouraged him to make a little more noise in order to continue clearing out his lungs. He responded with a few weak cries. Nothing very loud, but enough that the medical professionals in the room felt comfortable with his state. (At this point one of the nurses took the warmer back out of the room. When our families saw her, they asked if that meant he was here. She smiled and nodded and they erupted in cheers. Agatha said she could hear them even with the door closed. We love having such fun, supportive family.)
Sadly, I didn't bond with him immediately. The weariness of what my body had just gone through along with the numbing effect of the drugs in my system prevented me from forming a close bond from the get-go. Thankfully as I held him and looked at him I began to feel closer to him. It didn't take much time before I was irrevocably attached to this beautiful boy that had grown within me. However, his daddy was smitten with him from the moment he laid eyes on him. He turned the video camera on shortly after Caleb came out and can be heard saying, "He's so cute!" Jonathan experienced the rush of love and immense joy I had expected for myself, and I'm so glad for it. Daddy deserved a reward too, especially after how much he gave to support his wife.
Though the baby was out, I continued to feel uncomfortable pressure down south. I woozily asked Dr. Partida why that was, and she told me it was the placenta. My body wasn't ready to expel it just yet, and during the process of actually delivering Caleb I had suffered 2nd and 3rd degree tears, so she worked on stitching me up for about 10 minutes. Finally, in just a couple pushes, the placenta was out. She held it up for Jonathan and I to see and I was struck by how big it looked.
Caleb was weighed at 8lb 10oz and measured at 20 inches. As soon as I was completely stitched up and Caleb had been given a clean bill of health (his apgar scores were 6 and 8), the personnel gradually trickled out of the room until was just Agatha and our little family of three. She helped me get Caleb latched on to nurse for the first time, which unfortunately didn't go very well. I was still fully reclined and the angle was just awkward. (However, we went on to have an incredible breastfeeding relationship that lasted 18 months.) I snuggled Caleb while Jonathan ran down the hall to let the families know that mama and baby were fine and tell them Caleb's stats. I held him a while longer then Daddy had a chance to hold him for the first time. I took a picture of them and the love pouring out of his eyes as he gazed at his son is overwhelming. Agatha gave Caleb a bath and showed Jonathan how to put a diaper on him. (This really came in handy over the next few weeks when Jonathan changed almost all of Caleb's diapers. My "area" had gone through so much trauma that I wasn't able to get around very well and spent most of the time sitting on the blowup donut the hospital kindly gave me.) After about 3 hours from the time Caleb was born, once we got him comfortable and swaddled and me situated in bed, we decided it was time to introduce him to the rest of his family. Agatha volunteered to go out and get them for us. Jonathan held Caleb as they filed in and we shared his name for the first time. They took turns holding him and he was so alert during all of it, gazing right back at each of them. They stayed for a little while and then left to get some sleep (they had been up all night too). Jonathan and I were beyond fatigued. We turned off the lights in the room, Jonathan snuggled up on the window seat bed with Caleb, and we all finally got some much needed sleep.
16 hours of labor, 4 of that spent pushing, and finally the birth of our son. This was one of - if not the - most profound, life changing experiences of my life. I was permanently altered in a matter of seconds. The only way I could think to describe what it felt like to give birth and become a mother is that my own heart began living outside my body; wherever that baby boy was, I felt a string attaching me to him. I physically felt the draw toward him, and if he wasn't in the room with me I felt a sense of missing. I became hyper aware of wherever he was, like a honing radar. It's not as intense now as it was in the early weeks, but the draw is still there and I don't think that will ever change.
Not everything went exactly as we had hoped, but we achieved a vaginal birth and we all came through it just fine. I've learned from our experience what I want to do differently next time. However, I don't have regrets about Caleb's birth. I am so grateful for the consistent support of my loving rock of a husband, my amazing nurses (my postpartum nurses were as wonderful as Agatha, who returned as our night nurse the following night), and my fantastic doctor. She knows us well and truly cares for us. We feel like we've gotten the best of both worlds: the training and licensing of an MD for Jonathan, the relationship and care of a midwife for me.
It's a true challenge to try and put into words a milestone like having a baby, but I've done my best. There's so much more from the days and weeks following his birth that I don't want to forget, but the experience of birthing Caleb is most important. I know this is lengthy; I intended this so I could have the most detailed record possible. I know that as time passes it will become increasingly difficult to remember everything that happened that night, so these posts are my attempt to preserve the story of how our sweet boy came into the world.
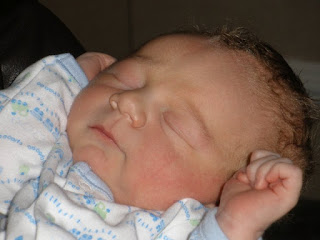
Caleb James Gilroy
3.28.10
8lb 10oz 20"